Create a free profile to get unlimited access to exclusive videos, sweepstakes, and more!
Doctors successfully treated a genetic disease in an unborn fetus
Just a little hardware update before release.
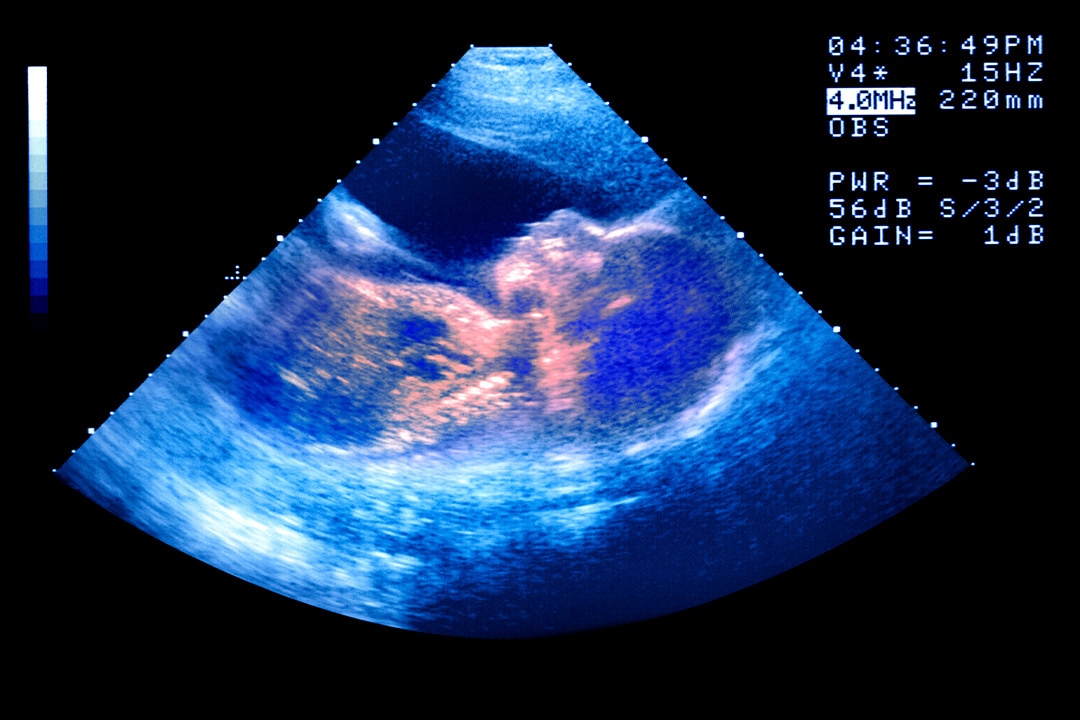
Pregnancy can be a time of intense emotions for everyone involved. Just revisit Knocked Up, Judd Apatow’s 2007 romantic comedy, by way of example. Seeing that little line on an at-home test or getting the first ultrasound can be among the happiest, and the most stressful, moments in a person’s life. It can also be one of the scariest, especially if you discover that your unborn child has a fatal disorder.
That was the situation for two parents from Ottawa. Twice before, they’d had children who died young — one at two years old and the other at 8 months — from a rare genetic disorder known as Infantile-Onset Pompe. Now they had another child on the way and a recent diagnose that it had Pompe too. They were staring down another tragedy unless someone could swoop in to save the day. That someone was Dr. Tippi MacKenzie, a pediatric surgeon at the University of California, San Francisco.
Dr. MacKenzie had previously treated fetuses with a hemoglobin disorder by giving them blood transfusions through the umbilical cord. The success of that practice got her thinking that a similar method might be used to treat fetal enzyme disorders. After success using the method in rats, the FDA suggested that Dr. MacKenzie begin a clinical trial in humans, targeting fetuses with enzyme disorders which had approved enzyme treatments.
RELATED: We cured pneumonia in mice by filling their lungs with swimming microrobots
Because of the family’s history, two previous children with Pompe, they knew to look for it and were enrolled in the trial. The results of that trial were recently published in The New England Journal of Medicine. The baby was born healthy and is about 16 months old at the time of this writing. Her parents named her Ayla and she’s developing normally, apparently undisturbed by the enzyme disorder which might have sent her along a very different path.
To understand how doctors pulled off a biological caper to save a life, we first have to talk about Infantile Onset Pompe. It affects fewer than one baby out of every 100,00, although it obviously gave this particular family more than their fair share. People with Pompe have low levels of certain enzymes, if they have measurable levels at all, which leads to a buildup of a type of sugar called glycogen. The result is weakening of the muscles and enlargement of the heart, which can stunt development and ultimately result in death.
In Pompe cases which emerge after birth, doctors can treat patients by providing the missing enzymes. That won’t undo any damage which has already happened, but it can prevent things from getting any worse. But when it happens early, before a person is even born, the disease tears through muscle fibers and thickens the heart before anyone knows there’s a problem. In Pompe and other lysosomal storage diseases, early diagnosis and treatment is crucial.
With that in mind, doctors decided to try enzyme replacement therapy while a fetus is still in the womb, in an attempt to prevent the disease from doing any damage at all. When Ayla’s mother was 24 weeks pregnant, they received their first dose of the enzyme, delivered straight to Ayla through the umbilical cord. Ayla and her mother received six doses in total, each spaced two weeks apart.
By all accounts, the treatment appears to have worked. Ayla was born without the signature heart problems associated with other Pompe babies, and she hasn’t had any delays in motor development which can be attributed to muscle damage.
Meanwhile, Ayla and her mother weren’t the only participants in the trial. By the time the paper was published, two other fetuses had been treated with this method and doctors reported that another of the babies was born on Oct. 27 following a pre-birth treatment for Hunter’s Syndrome. Doctors are monitoring his condition, according to The New York Times.
Admittedly, the sample size is small, and it will take years to see how the treatment shakes out long-term. But if it works, and it seems like it does so far, it could be a breakthrough for a collection of debilitating or fatal disorders.


























